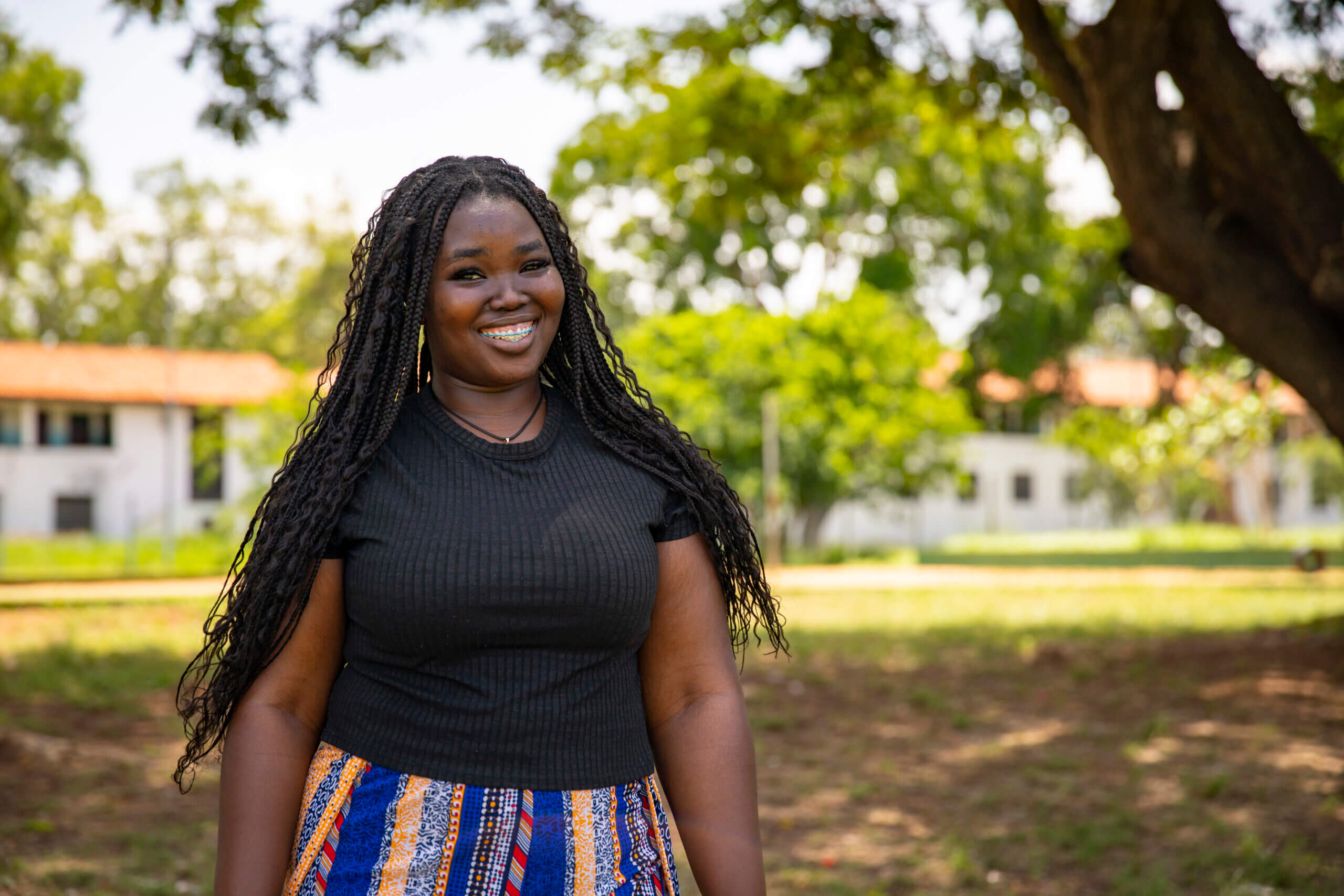Reproductive healthcare for people with disabilities
Worldwide, about 15% of people live with a disability. Like anyone else, they have a right to make their own choices about their bodies and futures. Yet, many are still denied access to reproductive healthcare. We must expand access to reproductive healthcare for people with disabilities.
At MSI, we’re committed to providing inclusive healthcare, and we’re overcoming the barriers that keep disabled people from accessing the care they need. Learn how we’re working to leave no one behind.
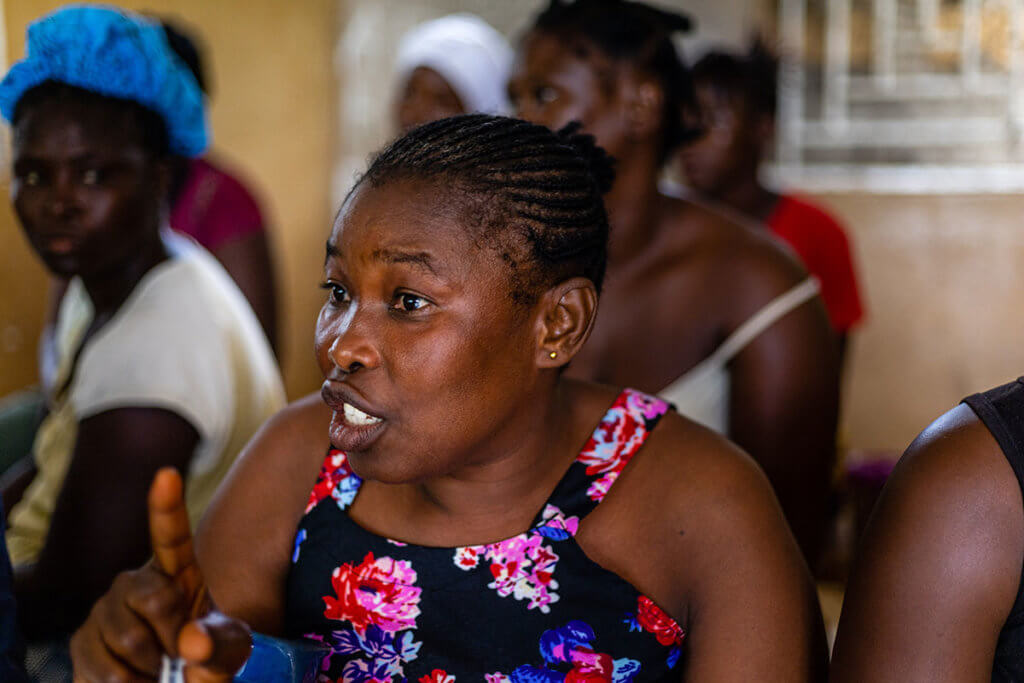
What barriers block reproductive healthcare for people with disabilities?
Women with disabilities have the same reproductive health needs as anyone else—from preventing unwanted pregnancies to routine care such as cervical cancer screenings. But healthcare providers and the broader community don’t always recognize these needs.
Even when healthcare providers understand that people with disabilities need reproductive healthcare, they might not provide services in a way that meet the disabled person’s needs. For example, a doctor who relies on written materials might fail to give adequate information to a blind client. Or, a doctor who’s used to moving quickly through appointments might not be able to hear the concerns of someone with speaking disabilities.
At MSI, we’re working to address these barriers—and we’re seeing the impact. In West and Central Africa, where we piloted our interventions, we increased service to people with disabilities tenfold. How did we do it? Here are three lessons we learned about providing more inclusive services.
1. Partner with organizations for people with disabilities to design inclusive services
Too often, the disabled community is excluded from program design. As a result, healthcare programs fail to meet the needs of the people they’re trying to serve. To change this, we partnered with local organizations for persons with disabilities, ensuring their insights directed the development of our programs.
In Sierra Leone, MSI worked with international and local partners to conduct community engagement workshops. In these workshops, we heard from people with disabilities about their experiences accessing reproductive healthcare. The feedback they gave us allowed us to adapt, making our services more inclusive.

Following the workshops, we came up with several interventions for MSI’s mobile outreach teams to test. One outcome was our Inclusive Services Guide, a handbook with useful information about how to best serve people with disabilities for outreach teams and providers. We also created “Rumor Cards”, which outreach teams and community-based mobilizers used to facilitate conversations about reproductive health for disabled people.
By educating our providers and the wider community, we improved the client experience. One woman with a disability told us: “They treated us like queens!”
2. Addressing social and cultural norms around disability
We’ve found that many people—from healthcare providers to neighbors in the community—hold misconceptions about the lives of people with disabilities.
We would have to challenge this misinformation if we wanted people with disabilities to feel comfortable coming to us for services. We began working to raise awareness about the range of services we offered. This included safe abortion where permitted, and the right to empowering care for all.
We worked with partners to develop a values clarification attitudes and transformation (VCAT) toolkit on disability inclusion for healthcare providers. This toolkit encouraged providers to explore any prejudices they may have around reproductive healthcare for people with disabilities. As a result, participants could recognize and address any negative assumptions or behaviors. .
We partnered with people with lived experience of disability to build awareness. One such woman was Zainab, our community-based mobiliser in Sierra Leone. Zainab is committed to building awareness of inclusive sexual and reproductive healthcare services. She’s made progress challenging harmful social norms. Zainab shared: “People with disabilities in my community now have the confidence to inquire and I can talk to them about services.”

3. Tailoring materials to be accessible
Finally, we reviewed our client-facing materials with an eye towards accessibility, including for low-literacy clients. to ensure that our materials were accessible and easy to read for people with a range of disabilities
We already tailored our client-facing materials for each country program’s unique cultural context. Now, we worked with partners to create guidance that would allow country programs to adapt their existing resources for people with disabilities.
The new guidance shared tips on adapting language and design to improve readability. It also covered the principles of creating “Easy-Read” resources. We encouraged teams to use visual imagery to help explain contraceptive options and potential side effects to clients who are unable to read.
With new materials in hand, we were able to better meet the needs of clients with disabilities. And with materials tailored to them, clients could feel more confident choosing the contraceptive method that made sense for them.