We can eliminate cervical cancer
In 2020, 342,000 women died of cervical cancer. Shockingly, nearly 90% of those deaths occurred in low- and middle-income countries. Women in these countries often lack access to preventative care, screening and treatment.
Fortunately, there are strategies available to eliminate this deadly disease. First, we can vaccinate girls with the HPV vaccine. Second, we can screen women regularly. Finally, we can offer treatment of abnormal cells early. Today, we’re sharing our progress toward ensuring access to this life-saving reproductive healthcare.
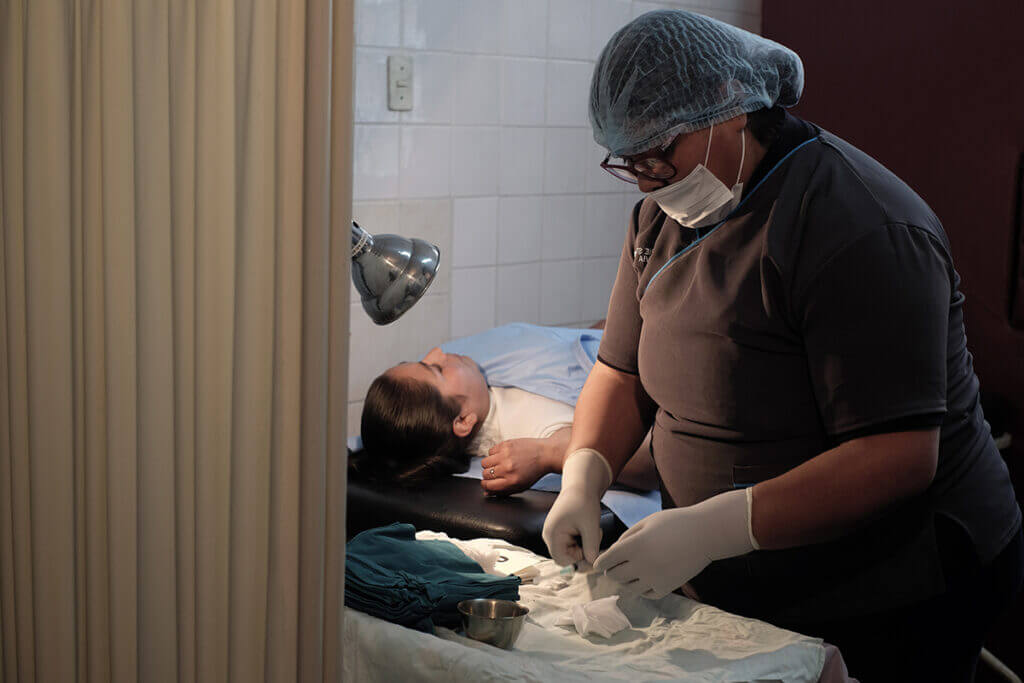
How we fight cervical cancer
The women we serve worry about cervical cancer. Many have heard of deaths in their community and want screening services that are convenient and affordable. That’s why we’re working to expand access to screening and treatment.
Across 24 of our country programs in sub-Saharan Africa and Asia, MSI provides cervical cancer prevention services through a variety of channels. These include our own centers or clinics, our network of socially franchised private clinics, as well as our mobile outreach teams and MSI Ladies. These trusted teams deliver services mainly in rural areas where there are little or no other health care services, going the last mile to ensure that every woman who wants it has access to choice.
Screening, prevention and treatment
The best way to end cervical cancer is to provide vaccines to girls 9-19, to prevent them from getting the most common strains of HPV that can lead to cancer. That’s why we offer HPV vaccines in several of our country programs. We hope to expand access to these vaccines even further in the future.
For women who haven’t been vaccinated, regular screenings in women age 30-49 can catch abnormal cells early. At MSI, we provide Visual Inspection with Ascetic Acid or VIA screening. This effective, inexpensive test allows healthcare workers to see potentially harmful lesions. Some country programs also offer HPV DNA tests. This test is similar to a Pap smear and identifies the forms of HPV most likely to lead to cancer. When abnormal cells are detected, many of our centers can provide treatment.
In 2022, MSI country programs delivered 209,513 cervical cancer screening and treatment services. That’s almost 800 women every single day receiving life-saving care.

Opening doors to reproductive health
Cervical cancer screening and treatment don’t just save lives. They open doors for women to access other forms of reproductive healthcare.
Many women who come for a cervical cancer screening take the opportunity to learn about contraception, HIV counseling and STI treatment. In Uganda, 77% of clients who came in for screening also accessed another service. The screening procedure helps dispel myths around contraception, IUDs in particular. Depending on location up to 65% of women who come in for a cervical cancer screening request a contraceptive method!
For the women we serve, getting screened for cervical cancer is often the first step towards learning more about contraception and other reproductive healthcare. Offering clients a “one-stop-shop” means a better experience and increased access to contraception.
Dr. Carole Sekimpi, our Uganda country director, reflected on the importance of these services. “Cervical cancer is one of the most common cancers in women. It is debilitating and deadly yet absolutely preventable through HPV vaccination, regular screening and early treatment. At MSUG we are committed to holistic care for the women we serve. This is why we have integrated cervical cancer screening, and early treatment in our service package. We observe that women hasten to the call for cancer screening, and about 25% of those screened also take up a family planning service during the same visit. The majority of these women will choose the IUD.”
Together, we can eliminate cervical cancer
Eliminating cervical cancer isn’t just a distant dream. It’s a real possibility. Together with our generous donors, MSI is doing our part to create a world where no woman dies of this preventable, treatable disease. We’ll continue innovating and expanding our reproductive healthcare options, so that every woman can access care no matter where she lives.